Many of our clients arrive after years, sometimes decades, of searching for answers.
They’ve worked with specialists, tried traditional treatment programs, and followed every recommended protocol, yet still find themselves stuck in cycles of pain, addiction, or emotional dysregulation that never fully resolve.
What sets us apart is not just the luxury setting or comprehensive services, but the way we integrate emerging neuroscience, somatic therapy, and pain recovery techniques into a cohesive, individualized plan, especially for clients whose symptoms don’t fit neatly into a diagnostic box.
We specialize in complexity: chronic pain that resists treatment, autoimmune issues, and nervous systems shaped by trauma, anxiety that starts in the body before it reaches the mind, and conditions that don’t respond to traditional methods. Our approach is built for those who have exhausted conventional options and are ready for something different. Something deeper.
This month, we’re sharing a case study that brings this approach to life. You’ll see how our polyvagal-informed treatment model helped a 50-year-old client with two decades of opioid use and chronic pain shift into measurable healing, physically, emotionally, and neurologically. It’s a clear example of how lasting change becomes possible when care is attuned to the body’s natural rhythms and readiness.
Our integrated residential program supports healing from trauma, addiction, and chronic pain by prioritizing safety, connection, and nervous system regulation. Rooted in polyvagal theory, our tiered model scaffolds care in alignment with each client’s physiological and emotional readiness.
A core goal of this approach is to improve daily functioning. Reducing depression, anxiety, disrupted sleep, and increasing social engagement so clients can reengage more fully in relationships, responsibilities, and meaningful living.
Case Spotlight
In a recent case*, a 50-year-old client with long-standing opioid use (no sustained sobriety since 2009), chronic pain, and unresolved trauma engaged in our program for 76 days.
At intake, he reported persistent lower back pain, especially in the mornings, with an average pain intensity of 5 to 6 out of 10. Treatment emphasized co-regulation, somatic tracking, pain reprocessing, and paced trauma work, grounded in the understanding that sustained recovery begins with safety.
Early Clinical Shifts (Days 1 to Day 21)
Measured using validated self-report tools, the client demonstrated significant early improvements:
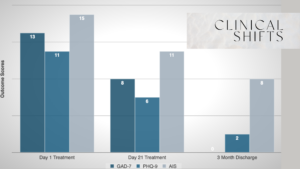
• GAD-7 (Anxiety): 13 → 8 (out of 21)
Reduction in internal mobilization and cognitive rumination
• PHQ-9 (Depression): 11 → 6 (out of 27)
Improved motivation, mood stability, and relational engagement
• AIS (Athens Insomnia Scale): 15 → 11 (out of 24)
Improved sleep quality, supporting restoration and daily rhythm
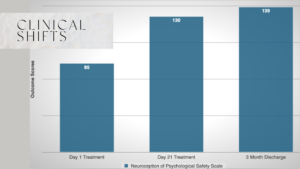
• NPSS (Neuroception of Safety Scale): 85 → 130 (out of 145)
Greater sense of emotional safety, trust, and co-regulation
In parallel, his pain narrative began to shift. With mind-body interventions and targeted psychoeducation, the client reported increased flexibility in how he related to physical sensations, describing early improvements in function and reduced distress related to pain.
Sustained Progress (3-Month Follow-Up)
Post-discharge assessments continued to reflect progress in regulation, safety, and integration:
• GAD-7 (Anxiety): 8 → 0 (out of 21)
• PHQ-9 (Depression): 6 → 2 (out of 27)
• AIS (Athens Insomnia Scale): 11 → 8 (out of 24)
• NPSS (Neuroception of Safety Scale): 130 → 139 (out of 145)
In his own words, regarding pain, at 3-Month Follow-Up:
“I’m 98% better. Zero or one pain level today. The ‘1’ is because I’m not a spring chicken anymore.”
Shared during a clinical follow-up, this sentiment reflects both pain recovery and the client’s growing sense of agency, humor, and embodied healing.
*All outcomes are collected confidentially and securely, with client consent.
We de-identify and share these results to offer insight into what’s possible when treatment honors the rhythm of healing.
Why This Matters
In polyvagal terms, these changes reflect a shift from states of defense to states of connection. By building capacity for safety and flexibility in the nervous system, clients are better able to access relationships, purpose, and long-term resilience. Pain, once central to the client’s identity and opioid use, became something that could be observed, understood, and managed without fear.
Importantly, the client has maintained sobriety, demonstrating how nervous system regulation supports sustained recovery in real life, not just in treatment.
What This Means for Clients, Families, and Professionals
This case is more than an individual success story; it’s a window into what becomes possible when we treat the nervous system as central to healing. For individuals living with pain or patterns that defy standard treatment, for families watching a loved one struggle without answers, and for professionals seeking new models for complex care, this outcome offers real hope.
It shows that recovery can begin in places medicine alone can’t reach. Through connection, safety, and the recalibration of the body’s stress response. At The Pointe Malibu, we meet complexity with curiosity, compassion, and combine rigorous clinical care with deeply attuned, neuroscience-informed practices.
Because when treatment honors the body’s natural rhythms and respects the full intricacy of a person’s experience, recovery doesn’t just happen, it lasts.
If this approach resonates with you, as a provider, a loved one, or someone seeking care, we welcome you to visit us in person. Stop by for a visit, We’d be honored to show you around.